Abstract
Background
Smoldering multiple myeloma (SMM) is an asymptomatic precursor condition to multiple myeloma (MM). Emerging data from clinical trials indicate that - compared to watchful monitoring - initiation of therapy at the SMM stage might be indicated. Currently, there is no established screening for SMM in the general population and therefore patients are identified incidentally. Here, we define for the first time, epidemiological and clinical characteristics of SMM in the general population based on a large (N>75,000) population-based screening study.
Methods
The iStopMM study (Iceland Screens Treats or Prevents Multiple Myeloma) is a nationwide screening study for MM precursors where all residents in Iceland over 40 years of age and older were invited to participate. Participants with a positive M-protein on serum protein electrophoresis (SPEP) or an abnormal free light chain (FLC) analysis entered a randomized controlled trial with three arms. Participants in arm 1 continued care in the Icelandic healthcare system as though they had never been screened. Arms 2 and 3 were evaluated at the study clinic with arm 2 receiving care according to current guidelines. In arm 3 bone marrow testing and whole-body low-dose CT (WBLDCT) was offered to all participants. SMM was defined as 10-60% bone marrow plasma cells on smear or trephine biopsy and/or M-protein in serum ≥3 g/dL, in the absence of myeloma defining events. Participants in arm 3 were used to estimate the prevalence of SMM as bone marrow biopsy was performed in all participants of that arm when possible. The age- and sex-specific prevalence was determined with a fitted function of age and sex, and interaction between those. Diagnosis at baseline evaluation of the individuals in the study was used to define the point prevalence of SMM.
Results
Of the 148,704 individuals over 40 years of age in Iceland, 75,422 (51%) were screened for M-protein and abnormal free light chain ratio. The 3,725 with abnormal screening were randomized to one of the three arms, and bone marrow sampling was performed in 1,503 individuals.
A total of 180 patients were diagnosed with SMM, of which 109 (61%) were male and the median age was 70 years (range 44-92). Of those, a total of 157 (87%) patients had a detectable M-protein at the time of SMM diagnosis with a mean M-protein of 0.66 g/dL (range 0.01-3.5). The most common isotype was IgG in 101 (56%) of the patients, 44 (24%) had IgA, 2 (1%) had IgM, and 5 (3%) had biclonal M-proteins. A total of 24 (13%) patients had light-chain SMM. Four patients (2%) had a negative SPEP and normal FLC analysis at the time of SMM diagnosis despite abnormal results at screening. A total of 131 (73%) patients had 11-20% bone marrow plasma cells at SMM diagnosis, 32 (18%) had 21-30%, 9 (5%) had 31-40%, and 8 (4%) had 41-50%. Bone disease was excluded with imaging in 167 (93%) patients (MRI in 25 patients, WBLDCT in 113 patients, skeletal survey in 27 patients, FDG-PET/CT in 1 patient), 13 patients did not have bone imaging performed because of patient refusal, comorbidities, or death.
According to the proposed 2/20/20 risk stratification model for SMM, 116 (64%) patients were low-risk, 47 (26%) intermediate-risk, and 17 (10%) high-risk. A total of 44 (24%) had immunoparesis at diagnosis. Using the PETHEMA SMM risk criteria on the 73 patients who underwent testing with flow cytometry of the bone marrow aspirates; 39 (53%) patients were low-risk, 21 (29%) patients were intermediate-risk, and 13 (18%) patients were high-risk.
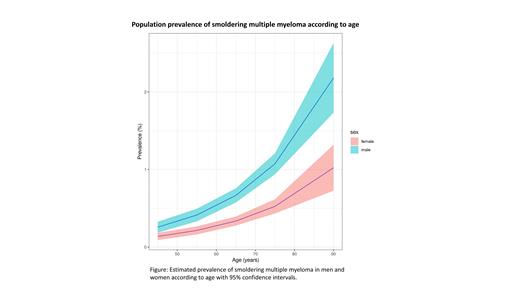
Out of the 1,279 patients randomized to arm 3, bone marrow sampling was performed in 970, and 105 were diagnosed with SMM (10.8%). The prevalence of SMM in the total population was estimated to be 0.53% (95% CI: 0.49-0.57%) in individuals 40 years of age or older. In men and women, the prevalence of SMM was 0.70% (95% CI: 0.64-0.75%) and 0.37% (95% CI: 0.32-0.41%), respectively, and it increased with age in both sexes (Figure).
Summary and Conclusions
Based on a large (N>75,000) population-based screening study we show, for the first time, that the prevalence of SMM is 0.5% in persons 40 years or older. According to current risk stratification models, approximately one third of patients have an intermediate or high risk of progression to MM. The high prevalence of SMM has implications for future treatment policies in MM as treatment initiation at the SMM stage is likely to be included in guidelines soon and underlines the necessity for accurate risk stratification in SMM.
Kampanis: The Binding Site: Current Employment. Hultcrantz: Daiichi Sankyo: Research Funding; Amgen: Research Funding; GlaxoSmithKline: Membership on an entity's Board of Directors or advisory committees, Research Funding; Curio Science LLC: Consultancy; Intellisphere LLC: Consultancy. Durie: Amgen: Other: fees from non-CME/CE services ; Amgen, Celgene/Bristol-Myers Squibb, Janssen, and Takeda: Consultancy. Harding: The Binding Site: Current Employment, Membership on an entity's Board of Directors or advisory committees, Patents & Royalties. Landgren: Janssen: Research Funding; Janssen: Other: IDMC; Celgene: Research Funding; Takeda: Other: IDMC; Janssen: Honoraria; Amgen: Honoraria; Amgen: Research Funding; GSK: Honoraria. Kristinsson: Amgen: Research Funding; Celgene: Research Funding.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal